How Metabolism Affects Weight Loss After 40: Complete Guide

Important Notice:This article is for informational and educational purposes only. The information provided does not replace guidance from a qualified healthcare professional. For personal decisions related to health, weight management, or supplementation, always consult a licensed physician or registered dietitian.
If you’ve been eating the same way you did at 30 but watching the scale creep upward anyway, you’re not imagining it — and you’re not alone. For millions of Americans over 40, weight loss suddenly feels like an uphill battle even when nothing about their habits has visibly changed. The reason is rooted in biology: metabolism, the intricate system your body uses to convert food into energy, shifts significantly as you age, and those changes have a direct, measurable impact on how your body stores and burns fat.
According to data from the National Institute on Aging, adults lose approximately 3–8% of their muscle mass per decade after age 30, with that rate accelerating after 60. Since muscle tissue is metabolically active — meaning it burns calories even at rest — this gradual loss has a compounding effect on resting metabolic rate (RMR). Research published in The Journal of Clinical Endocrinology & Metabolism found that RMR decreases by roughly 1–2% per decade in adults, which may not sound significant until you do the math: for a person who burns 1,800 calories at rest at age 30, that could translate to 200–400 fewer calories burned per day by their mid-50s.
Having worked alongside registered dietitians and exercise physiologists, and having reviewed dozens of clinical protocols for adult weight management, we’ve seen one pattern repeat itself consistently: the adults who successfully manage their weight after 40 are not the ones trying hardest on the treadmill — they’re the ones who understand and actively support their metabolism. This guide draws on that professional experience to give you a clear, evidence-based picture of what’s actually happening inside your body and what you can do about it.
By the time you finish reading, you’ll understand exactly how metabolism changes after 40, which lifestyle factors speed up or slow down those changes, and the most effective, sustainable strategies for working with your biology — not against it — to achieve and maintain a healthy weight for the long term.
You might like to know about: Health and Longevity After 40: A Complete and Reliable Guide
What Metabolism Actually Means — and Why It Changes After 40
The word ‘metabolism’ gets used casually in everyday conversation, but its clinical meaning is both more specific and more illuminating. Your metabolism is the sum of all chemical reactions your body uses to sustain life — converting nutrients into energy, repairing cells, regulating hormones, and maintaining organ function. When people talk about a ‘fast’ or ‘slow’ metabolism, they’re usually referring to resting metabolic rate (RMR): how many calories your body burns just to keep functioning while at rest.
The Four Components of Daily Calorie Burn
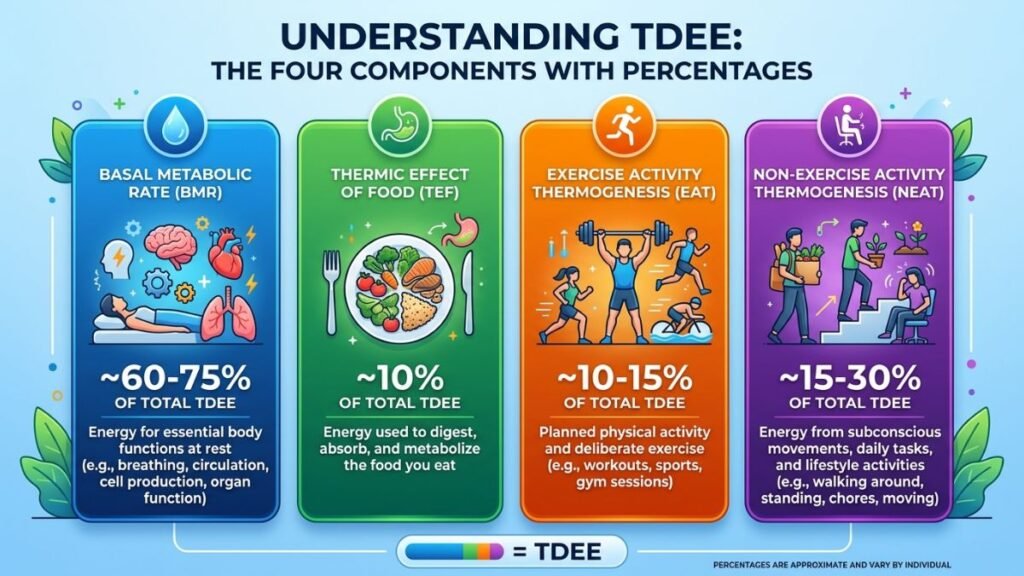
Your total daily energy expenditure (TDEE) is made up of four distinct components, and understanding how each one shifts with age is fundamental to understanding weight gain after 40:
- Resting Metabolic Rate (RMR): Accounts for 60–75% of all calories burned daily. Decreases steadily with age, primarily due to muscle loss and hormonal changes.
- Thermic Effect of Food (TEF): The energy required to digest, absorb, and process nutrients — roughly 10% of total intake. Protein has the highest thermic effect at 20–30%, compared to 5–10% for carbohydrates and 0–3% for fats.
- Non-Exercise Activity Thermogenesis (NEAT): Calories burned through daily movement that isn’t formal exercise — walking, fidgeting, household tasks. This is highly variable and tends to decline naturally as people become more sedentary with age.
- Exercise Activity Thermogenesis (EAT): Calories burned during deliberate exercise. This remains fully within your control at any age.
Why the 40s Mark a Turning Point
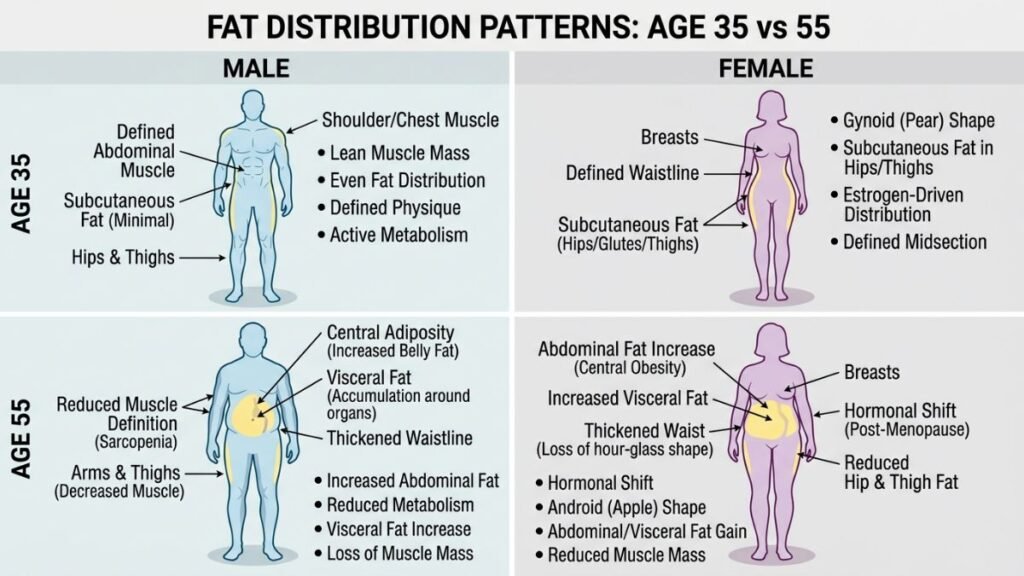
Age 40 represents a convergence of several biological processes that collectively suppress metabolic rate. Testosterone levels in men begin a measurable decline around age 35–40, with some studies noting a 1–2% decrease per year. Estrogen fluctuations in women approaching perimenopause alter fat distribution, shifting storage toward the abdomen. Growth hormone, which stimulates muscle synthesis and fat metabolism, decreases substantially in both sexes. Simultaneously, chronic low-grade inflammation — sometimes called ‘inflammaging’ — begins to interfere with insulin signaling, gradually impairing the body’s ability to efficiently use glucose for energy.
Taken together, these changes don’t mean weight loss becomes impossible after 40. They mean the strategies that worked at 25 may no longer be sufficient — and that new, more targeted approaches are warranted.
The Muscle-Metabolism Connection: Why Strength Training Becomes Non-Negotiable
Of all the factors that influence metabolic rate after 40, lean muscle mass is the most powerful and the most controllable. A single pound of muscle tissue burns approximately 6–10 calories per day at rest, compared to approximately 2 calories per pound of fat tissue. This may seem modest, but consider the compound effect: losing 10 pounds of muscle over a decade — a realistic scenario without intentional resistance training — can reduce your resting calorie burn by 60–100 calories per day, or 600–1,000 calories per week.
Sarcopenia: The Silent Metabolic Thief
The age-related loss of skeletal muscle mass and function has a clinical name: sarcopenia. The condition is far more common than most adults realize. According to the American Journal of Clinical Nutrition, sarcopenia affects an estimated 10–25% of people in their 60s and up to 50% of those over 80. But the process begins decades earlier, which is precisely why intervention in your 40s is so strategically important.
Sarcopenia doesn’t just reduce metabolic rate. It also impairs glucose uptake (muscle tissue is the primary site for insulin-driven glucose clearance), reduces bone density, increases fall risk, and diminishes functional independence. Addressing it through resistance training is arguably the single highest-return health investment available to adults over 40.
How to Build and Maintain Muscle After 40
The fundamentals of muscle maintenance after 40 are well-established. Research consistently supports:
- Progressive overload resistance training 2–4 times per week, prioritizing compound movements (squats, deadlifts, rows, pressing movements)
- Protein intake of 1.2–1.6 grams per kilogram of body weight per day, with meals spaced to include 25–40 grams of complete protein per sitting
- Adequate recovery time between sessions — muscle protein synthesis peaks 24–48 hours post-workout and requires rest to complete
- Creatine monohydrate supplementation, which has among the strongest evidence bases of any supplement for preserving and building muscle in older adults
| Practical Tip:If you’re new to strength training after 40, start with bodyweight exercises or machine-based resistance for the first 4–6 weeks to build foundational movement patterns and reduce injury risk. Working with a certified personal trainer for even a few sessions to establish form is one of the highest-value investments you can make in your long-term metabolic health. |
Hormones, Insulin Resistance, and Fat Storage After 40
No discussion of metabolism after 40 is complete without addressing the hormonal landscape — because hormones are essentially the operating system that governs how your body manages energy, hunger, fat storage, and muscle synthesis. Several hormonal shifts that occur in your 40s and 50s work in combination to make fat loss more challenging, particularly around the midsection.
Insulin Resistance: The Metabolic Bottleneck
Insulin is the hormone responsible for signaling cells to take up glucose from the bloodstream. As adults age and accumulate visceral fat, their cells become progressively less responsive to insulin — a condition called insulin resistance. The pancreas compensates by producing more insulin, but chronically elevated insulin levels actively promote fat storage and inhibit fat breakdown (lipolysis).
The result is a metabolic environment that favors fat accumulation even at calorie levels that previously maintained weight. The CDC estimates that approximately 38% of American adults have prediabetes — the preclinical stage of insulin resistance — many of whom are unaware. Regular blood glucose monitoring, annual HbA1c testing after 40, and lifestyle interventions that improve insulin sensitivity are therefore not optional extras but core components of metabolic health management.
Cortisol: The Stress-Fat Connection
Cortisol, the primary stress hormone, has a direct relationship with abdominal fat accumulation. Cortisol promotes glucose release into the bloodstream (a survival mechanism) and, in chronically elevated states, signals the body to store excess energy as visceral fat around the organs. For adults navigating the career, family, and financial pressures typical of midlife, chronic cortisol elevation is genuinely common — and genuinely metabolically consequential.
Practical cortisol management strategies with direct metabolic relevance include: consistent 7–9 hour sleep, regular moderate-intensity aerobic exercise (excessive high-intensity exercise can paradoxically raise cortisol), stress-reduction practices such as diaphragmatic breathing or mindfulness, and limiting caffeine intake after 12 PM.
Sex Hormones and Fat Distribution
The decline in estrogen during perimenopause and menopause shifts fat storage patterns in women from the hips and thighs toward the abdomen — a metabolically less favorable distribution because visceral fat is more metabolically active and inflammatory. For men, declining testosterone levels are associated with reduced muscle mass, increased fat mass, and lower energy expenditure. While hormone replacement therapies exist and are actively prescribed by physicians for these conditions, lifestyle modifications remain foundational regardless of hormonal treatment decisions.
Diet Strategy for Metabolic Health After 40: What the Research Actually Shows
Nutrition advice for adults over 40 is often identical to generic weight-loss guidance, which misses the metabolic-specific nuances that actually matter for this age group. The dietary approaches with the strongest evidence for supporting metabolic health after 40 share several common principles that differ from the calorie-counting models many adults grew up with.
Protein: The Most Important Macronutrient After 40
For adults over 40, protein is not just one macronutrient among three — it plays a uniquely important role in preserving muscle mass, supporting satiety, and maintaining a higher thermic effect of feeding. The Recommended Dietary Allowance (RDA) for protein of 0.8 g/kg/day was established primarily to prevent deficiency, not to optimize muscle health in aging adults. Leading sports nutrition researchers now recommend 1.2–1.6 g/kg/day as the target range for active adults over 40 — and up to 2.0 g/kg/day for those doing regular resistance training.
High-quality protein sources with complete amino acid profiles include lean poultry, fish, eggs, Greek yogurt, cottage cheese, and legumes combined with whole grains. Distributing protein intake evenly across meals — rather than concentrating it at dinner — has been shown to improve muscle protein synthesis rates.
| Best Practice:Aim to include 25–40 grams of complete protein at each main meal. This targets the ‘leucine threshold’ — the minimum amount of the amino acid leucine needed to maximally stimulate muscle protein synthesis. This approach typically means starting breakfast with eggs, Greek yogurt, or a protein shake rather than cereal or toast alone. |
Carbohydrates, Glycemic Load, and Metabolic Stability
The quality and timing of carbohydrate intake has meaningful metabolic consequences for adults over 40 dealing with declining insulin sensitivity. Rapidly digested carbohydrates — white bread, sweetened beverages, processed snacks — produce sharp blood glucose spikes followed by insulin surges, which promote fat storage and trigger subsequent hunger cycles. Replacing these with lower-glycemic-load options (legumes, vegetables, intact whole grains, berries) provides sustained energy without the same insulin-driven fat storage signals.
Time-restricted eating (TRE) — typically limiting food intake to an 8–10 hour window each day — has shown meaningful metabolic benefits in several clinical trials, including improvements in insulin sensitivity, reductions in visceral fat, and improvements in cardiometabolic markers. It is not a requirement for metabolic health, but it is a legitimate tool for adults who find it compatible with their lifestyle.
Foods That Support Metabolic Function After 40
- Fatty fish (salmon, sardines, mackerel): Omega-3 fatty acids reduce inflammatory markers and support insulin sensitivity
- Berries: High antioxidant content counters oxidative stress associated with metabolic dysfunction
- Cruciferous vegetables (broccoli, cauliflower, Brussels sprouts): Support liver detoxification pathways involved in hormone metabolism
- Green tea: Catechins and caffeine have a demonstrated modest thermogenic effect
- Extra-virgin olive oil: Oleic acid and polyphenols reduce inflammation and support healthy lipid profiles
- Fermented foods (yogurt, kefir, kimchi): Support gut microbiome diversity, which is increasingly linked to metabolic health
The table below summarizes how different lifestyle approaches compare across key metabolic health factors for adults over 40:
| Factor | Sedentary, No Diet | Diet Only | Exercise Only | Diet + Exercise |
|---|---|---|---|---|
| Muscle Mass | Declining fast | Moderate decline | Preserved/Built | Actively built |
| Resting Metabolic Rate | Lowest | Low | Moderate | High |
| Fat Burning Efficiency | Poor | Fair | Good | Very Good |
| Insulin Sensitivity | Low | Low-Mod | Moderate | High |
| Energy Levels | Fatigue common | Variable | Stable | Consistently high |
Exercise After 40: The Right Mix for Metabolic Optimization
Exercise remains the most powerful metabolic lever available to adults over 40 — but the type, frequency, and intensity of exercise that produces the best metabolic outcomes shift meaningfully with age. The traditional advice to ‘do more cardio’ to lose weight is an oversimplification that misses the most metabolically important categories of physical activity for midlife adults.
Resistance Training: Foundation of Metabolic Health
As established in the muscle-metabolism section, resistance training is non-negotiable for metabolic health after 40. The American College of Sports Medicine recommends that adults engage in resistance training targeting all major muscle groups at least twice per week. For metabolic optimization, three to four sessions per week is more effective, with workouts structured to progressively increase challenge over time.
Compound, multi-joint exercises — squats, hip hinges (deadlifts, Romanian deadlifts), rows, presses, and carries — produce greater hormonal responses, burn more calories, and develop functional strength more effectively than isolation exercises alone. A well-designed program should include both pushing and pulling movements, lower body and upper body emphasis, and progressive loading over weeks and months.
Cardiovascular Exercise: Zone 2 Training
For fat metabolism, cardiovascular training at moderate intensity — specifically ‘Zone 2’ training, which corresponds to roughly 65–75% of maximum heart rate — is particularly effective. Zone 2 exercise primarily burns fat as fuel, improves mitochondrial density (essentially the cellular machinery for fat oxidation), and enhances cardiovascular efficiency without the cortisol-raising effects of high-intensity work.
For practical purposes, Zone 2 feels like a pace at which you can hold a conversation but not comfortably sing. Walking briskly, cycling at moderate effort, swimming, or using an elliptical all qualify. Thirty to 45 minutes, four to five times per week, is a well-supported Zone 2 target for adults over 40.
| Attention:High-intensity interval training (HIIT) is frequently recommended for metabolism, and it does have genuine benefits — particularly for insulin sensitivity and cardiovascular fitness. However, for adults over 40, overuse of HIIT can elevate cortisol chronically, impair recovery, and increase injury risk. A balanced program typically includes 1–2 HIIT sessions per week maximum, supported by a larger base of Zone 2 cardiovascular work and consistent resistance training. |
NEAT: The Underestimated Metabolic Variable
Non-Exercise Activity Thermogenesis (NEAT) — the calories burned through daily movement outside of formal exercise — can account for a significant metabolic difference between individuals. Research from the Mayo Clinic has found that NEAT varies by up to 2,000 calories per day between individuals of similar body size. Sedentary desk jobs, increased screen time, and more convenient transportation options all reduce NEAT progressively over midlife.
Practical NEAT-increasing strategies include: standing desks or walking workstations, taking stairs consistently, parking farther away, walking during phone calls, and setting movement reminders to break up prolonged sitting (every 45–60 minutes). These behaviors cumulatively can add 200–500 calories of daily energy expenditure without any formal exercise.

Sleep, Stress, and the Overlooked Drivers of Metabolic Health
Many adults over 40 focus exclusively on diet and exercise when addressing metabolism, overlooking two factors that can undermine even the most disciplined nutritional and training approach: sleep quality and chronic stress. Both have direct, well-documented effects on metabolic rate, hormone regulation, appetite control, and body composition.
Sleep as a Metabolic Regulator
Sleep is not passive recovery time — it is an active metabolic process during which growth hormone is secreted, muscle protein synthesis occurs, cortisol is regulated, and appetite-controlling hormones are balanced. Research consistently shows that sleeping fewer than 7 hours per night:
- Increases ghrelin (hunger hormone) by 14–28%, driving increased appetite
- Decreases leptin (satiety hormone) by 15–26%, impairing fullness signaling
- Elevates cortisol, promoting visceral fat accumulation
- Reduces insulin sensitivity, mimicking pre-diabetic metabolic states
- Impairs recovery from exercise, reducing the metabolic benefits of training
For adults over 40, sleep architecture also changes: deep, slow-wave sleep decreases, and sleep fragmentation becomes more common. Sleep hygiene interventions with strong evidence include: consistent sleep and wake times (including weekends), limiting screen exposure 60–90 minutes before bed, keeping the bedroom cool (65–68°F is well-supported), and avoiding alcohol within 3 hours of sleep (alcohol disrupts REM and slow-wave sleep despite feeling sedating).
Chronic Stress Management as Metabolic Medicine
The relationship between psychological stress and metabolic dysfunction is bidirectional and well-established. Chronic activation of the hypothalamic-pituitary-adrenal (HPA) axis — the physiological stress response system — elevates cortisol, disrupts insulin signaling, promotes inflammation, and reliably increases abdominal fat storage.
Evidence-based stress management techniques with documented metabolic benefits include regular moderate aerobic exercise, mindfulness-based stress reduction (MBSR), diaphragmatic breathing practices, time in natural environments, and social connection. These interventions are not soft additions to a metabolic health program — they are core components with measurable physiological effects.
| Practical Tip:A straightforward daily practice: spend 10 minutes each morning doing slow, diaphragmatic breathing (inhale for 4 counts, hold for 2, exhale for 6). This activates the parasympathetic nervous system, measurably reduces morning cortisol, and takes less than 15 minutes to implement. Over 8 weeks, practitioners consistently report improvements in sleep quality, energy levels, and reduced cravings for high-sugar foods — all of which have direct metabolic relevance. |
A Practical Step-by-Step Protocol for Metabolic Reset After 40
Theory without application has limited value. The following protocol synthesizes the evidence reviewed in this guide into a concrete, sequential approach that adults over 40 can implement progressively. This is not a crash program — it is a sustainable lifestyle architecture designed for long-term results.
- Get your baseline metrics. Before changing anything, schedule blood work to assess fasting glucose, HbA1c, insulin, thyroid function (TSH, free T3/T4), testosterone or estrogen (as appropriate), vitamin D, and a complete metabolic panel. Knowing your actual hormonal and metabolic starting point removes guesswork from the process.
- Establish protein targets. Calculate your body weight in kilograms (pounds ÷ 2.2) and multiply by 1.4 to find your daily protein target in grams. Begin tracking intake using an app or food journal for the first 2–4 weeks until you develop reliable intuition for meeting the target.
- Start resistance training twice per week. In the first month, focus on learning movement patterns rather than loading. A simple full-body program with 3–4 compound exercises per session, 3 sets of 8–12 repetitions, performed consistently, outperforms complex programs done inconsistently.
- Optimize sleep first. Before adding morning workouts or dietary restriction, ensure you are consistently sleeping 7–8 hours. Address sleep quality issues through the hygiene interventions described above. This single change often produces noticeable improvements in energy, appetite control, and body composition within 2–3 weeks.
- Add daily walking. Aim for 7,000–10,000 steps per day as a NEAT baseline. A simple pedometer or phone step counter is sufficient. Walking is broadly accessible, cortisol-neutral, and metabolically meaningful at cumulative daily volumes.
- Adjust carbohydrate quality. Replace refined carbohydrates (white bread, sweetened beverages, processed snacks) with lower-glycemic alternatives. This does not require eliminating carbohydrates — it requires choosing forms that produce smaller insulin responses and greater satiety per calorie.
- Review and adjust every 8 weeks. Metabolism is not a static system — it adapts to interventions. Every 8 weeks, reassess: Are you progressively increasing resistance in training? Is protein intake consistent? Has sleep quality stabilized? Adjust the most lagging variable before adding complexity.
Common Mistakes That Undermine Metabolism After 40 — and How to Avoid Them
Even well-intentioned adults frequently make a set of consistent errors when attempting to improve metabolic health after 40. Recognizing these patterns is as important as implementing the right strategies.
Mistake 1: Aggressive Calorie Restriction
Severely cutting calories — below 1,200 calories per day for women or 1,500 for men — may produce short-term weight loss, but it reliably triggers adaptive thermogenesis: the body reduces its metabolic rate in response to perceived food scarcity. This metabolic adaptation can persist for years after a diet ends, which is the physiological basis of ‘yo-yo dieting.’ For adults over 40, severe calorie restriction also accelerates muscle loss, directly worsening the metabolic foundation.
A more effective approach: aim for a moderate caloric deficit of 300–500 calories per day, prioritize protein to preserve muscle, and use resistance training as a core component. This produces slower but more sustainable fat loss with far less metabolic adaptation.
Mistake 2: Ignoring Recovery
The drive to exercise more when results stall is understandable but often counterproductive. More exercise without adequate recovery increases cortisol, impairs muscle protein synthesis, disrupts sleep, and can lead to overtraining syndrome — a genuine clinical state characterized by persistent fatigue, mood disruption, and paradoxically reduced performance. For adults over 40, recovery capacity decreases compared to younger adults, making 1–2 full rest days per week a performance and metabolic strategy, not laziness.
Mistake 3: Relying Solely on Cardio
Cardiovascular exercise is valuable, but over-relying on it while neglecting resistance training leaves the most powerful metabolic lever — muscle mass — unused. Many adults over 40 who exercise regularly but remain frustrated with body composition changes are doing substantial amounts of cardio with minimal resistance training. Rebalancing toward 2–4 strength sessions per week, supplemented by cardio, typically produces dramatically better body composition outcomes than cardio alone.
| Attention:If you have been doing the same type of exercise for more than 3 months with diminishing results, your body has adapted to that stimulus. Metabolic adaptation to exercise is real and well-documented. Introducing new stimuli — heavier loads, different movement patterns, or altered training frequency — is not optional variety; it is a physiological requirement for continued progress. |
Putting It All Together: Your Metabolism Is Not Fixed

The central message of this guide is one that runs counter to a great deal of popular discourse about aging and metabolism: your metabolic rate after 40 is not a predetermined sentence. It is a dynamic, responsive system that responds — measurably and meaningfully — to the inputs you provide consistently over time.
The key actionable takeaways from everything covered here:
- Muscle mass is the primary driver of resting metabolic rate, and resistance training is the most effective tool for building and preserving it after 40.
- Hormonal changes — declining sex hormones, rising cortisol, and developing insulin resistance — are real metabolic forces that respond to targeted lifestyle interventions including dietary quality, exercise type, sleep, and stress management.
- Diet strategy after 40 must prioritize adequate protein (1.2–1.6 g/kg/day), reduce refined carbohydrate load, and emphasize anti-inflammatory food quality over simple calorie counting.
- Sleep and stress are not secondary lifestyle factors — they are core metabolic inputs with quantifiable effects on hormone balance, fat storage, and exercise response.
Metabolic health after 40 is not about restriction, punishment, or heroic effort. It is about building a system — a set of daily practices — that works with your biology rather than fighting it. The adults who sustain healthy body composition and energy levels into their 50s, 60s, and beyond are not the ones who found more willpower. They are the ones who built better habits.
Start with one change this week. Add protein to breakfast. Begin a twice-weekly strength training routine. Commit to a consistent sleep window. Small, consistent actions compound into substantial metabolic transformation over months and years — and your 40s are an excellent time to begin.
If you found this guide useful, bookmark it for reference, share it with someone navigating similar challenges, or leave a comment with your experience — your questions and insights help us create better resources for everyone on this journey.
Frequently Asked Questions About Metabolism and Weight Loss After 40
How long does it take to see metabolic changes after starting exercise?
Most people notice measurable changes in energy and endurance within 4–6 weeks of consistent aerobic and strength training. Significant improvements in resting metabolic rate typically appear after 8–12 weeks, as muscle mass increases. Hormonal markers such as insulin sensitivity can begin improving within as little as 10 days of daily moderate exercise, even before body composition visibly changes.
Can metabolism actually be ‘fixed’ after 50?
Yes — the metabolic slowdown associated with aging is largely reversible through the right lifestyle interventions. Studies from institutions like the Harvard T.H. Chan School of Public Health confirm that progressive resistance training, adequate protein intake, and stress management can meaningfully restore metabolic rate in adults over 50. It takes consistency, but the biological machinery for improvement remains intact well into your 60s and beyond.
Is intermittent fasting safe for people over 40?
For most healthy adults over 40, time-restricted eating (such as a 16:8 schedule) is generally safe and can support metabolic health. However, women in perimenopause or menopause may find that extended fasting disrupts cortisol and estrogen balance. Anyone with a history of disordered eating, diabetes, or thyroid conditions should consult a physician before starting. The approach works best when combined with nutrient-dense meals, not used as a shortcut to calorie restriction.
What is the single most impactful change someone over 40 can make for metabolism?
Building and preserving lean muscle mass through resistance training is the highest-leverage intervention for metabolic health after 40. Muscle tissue burns approximately 6–10 calories per pound per day at rest, compared to about 2 calories for fat tissue. Even two 30-minute strength sessions per week can meaningfully raise your resting metabolic rate, improve insulin sensitivity, and support bone density simultaneously.
Does drinking more water actually boost metabolism?
Research shows that drinking approximately 17 oz (500 ml) of cold water can temporarily increase metabolic rate by 24–30% for 30–60 minutes. Over a day, adequate hydration (typically 8–10 cups for adults) supports enzymatic processes involved in fat metabolism, digestion, and detoxification. While water alone is not a magic solution, chronic mild dehydration demonstrably slows metabolic function — so consistent intake is a legitimate and low-cost metabolic support strategy.
How does sleep affect weight loss and metabolism after 40?
Sleep is one of the most underestimated metabolic regulators. Consistently sleeping fewer than 7 hours per night elevates ghrelin (the hunger hormone) and suppresses leptin (the satiety hormone), driving increased caloric intake by an average of 300–500 extra calories per day. Poor sleep also elevates cortisol, which promotes fat storage — particularly visceral (abdominal) fat. Adults over 40 who prioritize 7–9 hours of sleep typically see better results from diet and exercise than those who don’t, all else being equal.
Are metabolism-boosting supplements worth it for people over 40?
Most over-the-counter supplements marketed as ‘metabolism boosters’ have modest clinical evidence at best. Exceptions include creatine monohydrate, which has strong research support for preserving and building muscle mass; magnesium, which supports over 300 enzymatic reactions including those involved in energy production; and vitamin D, deficiency of which is associated with reduced metabolic efficiency. Before purchasing any supplement, a blood panel with your physician will reveal actual nutritional gaps rather than guesswork.