Why Is It So Hard to Lose Weight After 40? (The Real Reasons)
This content is for informational and educational purposes only. It does not constitute medical advice. Please consult your healthcare provider before making changes to your diet, supplements, or health routine.
Weight loss after 40 is genuinely harder — not because you’ve lost willpower or discipline, but because your body has changed in ways that most conventional diet advice completely ignores.
You’re eating the same things you always did. Maybe even less. You’re exercising, managing your life, doing your best. And yet the scale barely moves — or worse, it climbs. The frustration is real, and so is the biology behind it.
According to the National Institute on Aging, the body undergoes significant shifts in metabolism, hormone production, and muscle composition beginning in the fourth decade of life — changes that have a direct impact on how easily you gain or lose weight. A landmark 2021 study published in Science by researchers at Duke University found that while true metabolic slowdown is more gradual than once believed, the combination of hormonal changes, muscle loss, disrupted sleep, and chronic stress creates a compounding effect that makes weight management genuinely more difficult after 40.
This article breaks down exactly what is happening inside your body — the metabolic, hormonal, and physiological shifts that change the rules — and which evidence-based strategies actually work when your body is no longer playing by the same rules it did at 28.
No outdated myths. No miracle promises. Just clear, honest science and strategies that respect your intelligence and your lived experience.
Your Metabolism After 40: What the Science Actually Says
The first thing most people blame for midlife weight gain is a “slow metabolism” — and while there is truth here, the full picture is more nuanced than most articles suggest.
Your basal metabolic rate (BMR) — the number of calories your body burns at rest — does decline with age. Research suggests this decline is roughly 1–2% per decade after age 30, translating to approximately 100–200 fewer calories burned per day by your mid-40s compared to your 20s.
That may not sound significant. But compounded over years, without any adjustment in eating habits, it adds up to real, measurable weight gain.
The Metabolic Slowdown Is Real — But Not the Whole Story
The Duke University study mentioned earlier found something surprising: resting metabolic rate stays relatively stable from age 20 to 60. The real metabolic decline accelerates after 60. So why does weight gain accelerate specifically in the 40s?
The answer lies in what is simultaneously happening to your body composition — the gradual and largely invisible loss of muscle tissue, shifting hormone levels, and changes in how your body handles stress, sleep, and blood sugar. These forces don’t operate in isolation. They reinforce each other.
NEAT: The Hidden Daily Energy Drop
NEAT — non-exercise activity thermogenesis — refers to all the calories you burn through everyday movement: walking around, standing, doing household tasks, fidgeting, climbing stairs. Research shows NEAT can account for 15–50% of total daily energy expenditure.
After 40, NEAT tends to decline quietly. You take the elevator more often. You sit longer at a desk. Your joints ache slightly, so you move less without consciously deciding to. These micro-reductions in daily movement are practically invisible — and yet they can account for several hundred calories less burned each day.
The Hormonal Shift That Rewires Your Body

If metabolism is the engine, hormones are the fuel system. After 40, that fuel system undergoes a significant overhaul — and the effects on body weight and fat distribution are profound.
Estrogen, Progesterone, and Where Fat Goes (Women)
For women, the late 30s and 40s bring perimenopause — a transition that can span 7–10 years before menopause arrives. During this period, estrogen levels fluctuate widely before declining. This has direct, measurable effects on body composition.
Estrogen plays a key role in directing where your body stores fat. When estrogen drops, fat storage shifts from the hips and thighs — the classic female pattern — to the abdomen. This is why many women notice not just more weight in their 40s, but weight in a different location. The body shape itself changes.
Visceral fat — fat stored around internal organs in the abdominal region — is not inert. It actively releases inflammatory compounds, disrupts insulin sensitivity, and significantly raises the risk of cardiovascular disease and type 2 diabetes. This makes it more than a cosmetic concern.
Progesterone decline, which often precedes significant estrogen changes, contributes to water retention, bloating, and sleep disruption — all of which further complicate weight management.
Testosterone and the Male Side of the Equation
Men are not exempt from hormonal changes. Testosterone levels decline at approximately 1–2% per year after age 30. By the mid-40s, many men experience measurable reductions in lean muscle mass, increases in belly fat, and slower recovery from physical activity.
Testosterone is critical for building and maintaining muscle tissue. Less muscle means a lower resting metabolic rate, reduced metabolic flexibility, and a greater tendency to store excess calories as fat rather than use them for energy.
Thyroid Function: The Commonly Missed Variable
Thyroid disorders — particularly hypothyroidism — become significantly more prevalent after 40, especially in women. An underactive thyroid slows nearly every metabolic process in the body, including calorie burning, fat mobilization, digestion, and energy production.
The symptoms of low thyroid function — fatigue, unexplained weight gain, brain fog, cold intolerance, dry skin, and low mood — are often dismissed as “just getting older.” This is why a TSH (thyroid-stimulating hormone) blood test should be a standard part of any midlife health workup, particularly if weight changes feel inexplicable.
⚠️ Attention: If you’re gaining weight despite no significant changes in diet or activity, and you also feel persistently tired, cold, or mentally foggy, ask your doctor to specifically test your thyroid function. Hypothyroidism is highly treatable and far more common than most people realize.
Sarcopenia: Losing Muscle Without Knowing It
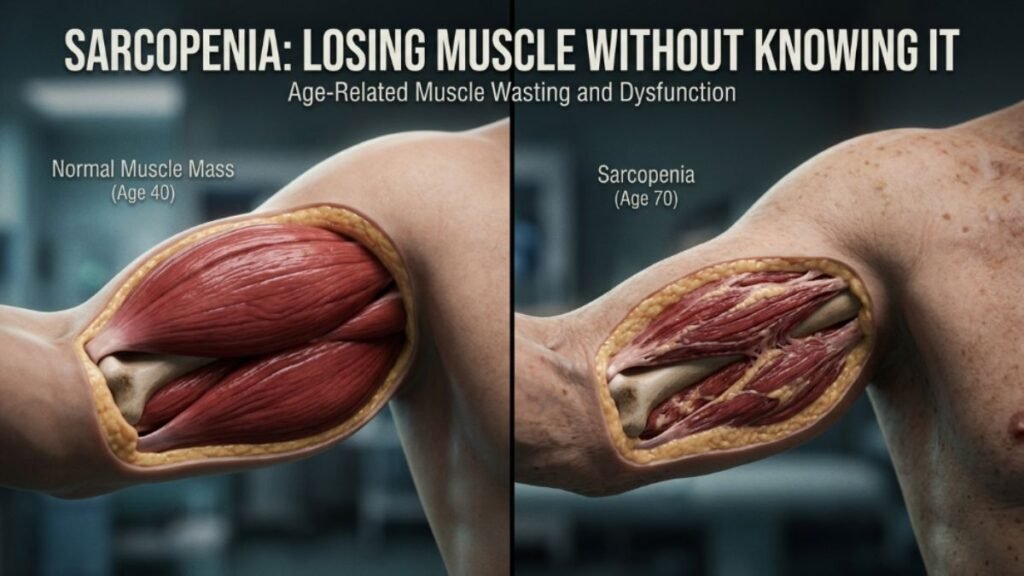
Sarcopenia — the medical term for age-related muscle loss — begins earlier than most people expect. The process starts in your 30s and accelerates after 40.
Research estimates adults lose approximately 3–8% of their muscle mass per decade after age 30. This rate increases further after 60. By midlife, many people have lost enough muscle to meaningfully reduce their resting metabolic rate — without any visible change on the scale.
Here is why this matters so much for weight management:
- Muscle is metabolically active tissue. Each pound of muscle burns approximately 6–10 calories per day at rest.
- Fat tissue, by contrast, burns almost no calories at rest.
- As muscle is silently replaced by fat — even if your total body weight remains unchanged — your daily calorie burn drops.
This is one reason the scale can be so misleading at midlife. You may weigh exactly what you weighed at 35, while your body composition has shifted in a direction that makes weight loss progressively harder.
The most effective single intervention against sarcopenia is progressive resistance training. Not cardio. Not yoga alone. Lifting progressively heavier weights signals your body to maintain and build muscle — and this remains highly effective well into your 50s and 60s.
👉 For a complete guide to metabolic support strategies, read our article on:
How to Boost Metabolism After 40
Cortisol and the Stubborn Belly Fat Connection
Modern midlife is rarely low-stress. Career demands, aging parents, financial pressures, family responsibilities — the mental and emotional load is heavy. And your body responds to all of it with cortisol.
Cortisol is your primary stress hormone. In short, acute bursts, it’s functional — it mobilizes energy and sharpens focus in response to a challenge. But when cortisol is chronically elevated, as it commonly is in busy 40-somethings, it becomes a powerful driver of fat storage.
Research consistently links elevated cortisol with increased visceral fat accumulation, particularly in the abdominal region. Cortisol does several things simultaneously that undermine weight management:
- Stimulates appetite and increases cravings for calorie-dense foods, especially sugars and refined carbohydrates
- Slows the breakdown of stored body fat
- Promotes fat storage, especially in the midsection
- Disrupts sleep quality, which further elevates cortisol the following day
The cortisol-belly fat loop is particularly hard to interrupt because its causes are deeply intertwined with the demands of midlife itself.
💡 Practical Tip: Chronic stress is not just uncomfortable — it is a biological barrier to weight loss. Stress management practices — whether meditation, regular movement, therapy, time in nature, or simply protecting better sleep — are not optional extras in your plan. They are core metabolic interventions.
Sleep Disruption and Weight Gain: The Connection Most Diets Ignore
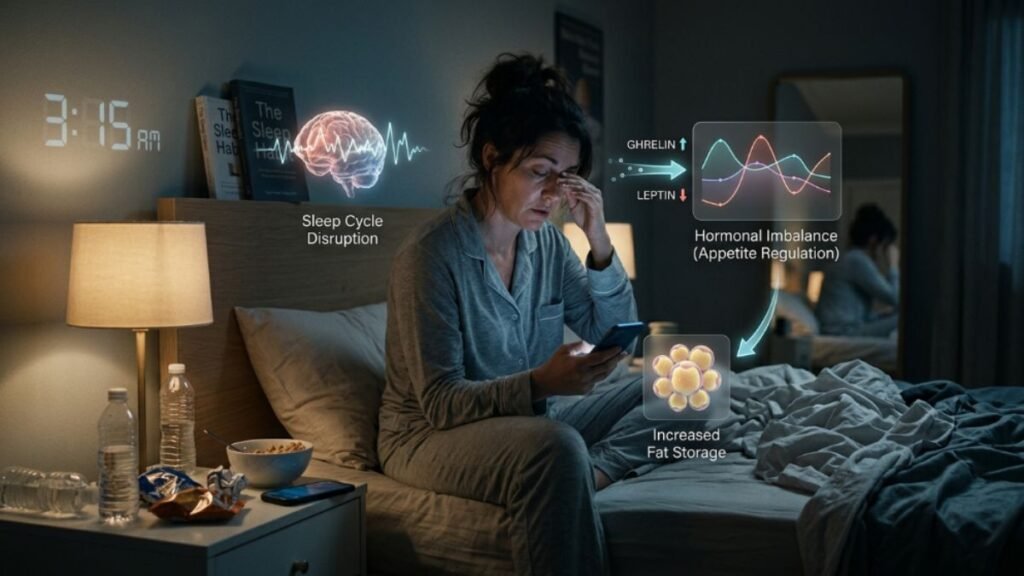
Sleep quality commonly deteriorates after 40. Hormonal fluctuations, heightened stress, and early-stage sleep apnea all contribute to fragmented, non-restorative sleep. And inadequate sleep has a direct, well-documented impact on weight and appetite.
Research consistently shows that sleeping fewer than 7 hours per night is associated with:
- Elevated ghrelin (the hunger-signaling hormone), increasing overall appetite
- Reduced leptin (the satiety hormone), delaying the feeling of fullness
- Higher cortisol levels the following day
- Stronger cravings for high-calorie, high-carbohydrate foods
- Reduced impulse control and poorer food decision-making
A 2022 study published in Obesity found that adults who extended their nightly sleep from under 6.5 hours to 8.5 hours consumed an average of 270 fewer calories per day — with no dietary intervention of any kind.
Sleep is not passive recovery time. It is when your body regulates hormones, repairs tissue, consolidates metabolic signaling, and resets the appetite system. Treating it as optional is one of the most expensive choices you can make when working on weight management after 40.
Insulin Resistance: The Hidden Driver Nobody Mentions
Insulin resistance is one of the most common — and most underdiagnosed — contributors to midlife weight gain. Yet it rarely appears in mainstream weight loss conversations.
Insulin is the hormone that enables your cells to absorb glucose (sugar) from the bloodstream for energy. When cells become resistant to insulin’s signal, the pancreas produces more of it to compensate. Higher circulating insulin levels signal the body to store fat and actively block fat burning.
Over time, insulin resistance contributes to:
- Difficulty losing weight despite caloric restriction
- Energy crashes after meals
- Persistent belly fat that resists conventional dieting
- Strong cravings for sweets and refined carbohydrates
- Elevated risk of metabolic syndrome and type 2 diabetes
Several factors that are common after 40 accelerate insulin resistance: sedentary behavior, chronic stress, poor sleep quality, and dietary patterns high in processed carbohydrates. Visceral fat itself produces inflammatory compounds that worsen insulin sensitivity — creating a self-reinforcing cycle.
The good news is that insulin resistance is largely reversible through lifestyle changes, particularly progressive resistance training, improvements in dietary quality, and better sleep.
✓ Best Practice: Standard blood tests measure fasting glucose, but fasting insulin is more sensitive as an early marker. Ask your doctor to include fasting insulin in your next metabolic panel — elevated insulin can exist alongside a normal glucose reading and is a much earlier warning signal.
👉 Certain evidence-based supplements may also support your efforts — see our guide to:
Natural Supplements for Adults Over 40: What Actually Works
What Actually Works: Evidence-Based Strategies for Weight Loss After 40

Understanding the challenges is essential. But the purpose of understanding them is to change your approach — to work with your biology rather than against it using tools designed for a 25-year-old’s body.
Here is what the evidence consistently supports for weight loss after 40:
1. Prioritize Protein at Every Meal
Protein offers several advantages that are especially relevant after 40:
- It preserves muscle mass during a caloric deficit, protecting your metabolic rate
- It has the highest thermic effect of all macronutrients — your body burns significantly more calories digesting protein than carbohydrates or fat
- It promotes satiety, naturally reducing total calorie intake without aggressive restriction
Research suggests a protein target of 1.2–1.6 grams per kilogram of body weight daily for active adults over 40. For a 160-pound (72 kg) adult, this means roughly 86–115 grams of protein per day — considerably more than the average American diet provides.
2. Resistance Training Is Non-Negotiable
Cardiovascular exercise has clear cardiovascular benefits, but it does not address sarcopenia or meaningfully rebuild metabolic capacity. Progressive resistance training — lifting progressively heavier loads over time — is the most important exercise modality for midlife weight management.
Aim for 2–3 sessions per week targeting all major muscle groups. A gym is not required. Bodyweight exercises, resistance bands, and dumbbells all produce meaningful results when applied consistently.
3. Reduce Ultra-Processed Foods and Refined Carbohydrates
A dietary pattern built around whole foods — lean proteins, healthy fats, complex carbohydrates, and abundant vegetables — directly addresses insulin resistance, reduces systemic inflammation, and supports hormonal balance.
You do not need to count every calorie. But reducing ultra-processed foods, which are specifically engineered to override your body’s natural satiety signals, makes every other strategy more effective.
4. Treat Sleep as a Metabolic Priority
Seven to nine hours of quality sleep per night is not optional when working on weight management after 40. If you are consistently sleeping fewer than 7 hours, addressing sleep quality should be your first intervention — before changing your diet.
5. Manage Stress as a Biological Strategy
Regular stress reduction practices — meditation, breathwork, physical movement, protecting boundaries, social connection, time outdoors — reduce cortisol over time, support hormonal balance, and remove one of the most significant invisible barriers to weight loss at midlife.
6. Recalibrate Your Timeline Expectations
Weight loss after 40 is typically slower than it was in your 20s or 30s. This is not failure. This is biology. A sustainable rate of 0.5–1 pound per week is not only realistic — it is the rate most associated with long-term success and muscle preservation.
| Strategy | Primary Benefit | Frequency |
|---|---|---|
| Resistance training | Preserves muscle, raises BMR | 2–3x per week |
| Adequate protein (1.2–1.6g/kg) | Muscle retention, satiety | Every meal |
| 7–9 hours sleep | Appetite regulation, cortisol control | Nightly |
| Stress management | Reduces cortisol-driven fat storage | Daily practice |
| Whole foods, reduced ultra-processed | Insulin sensitivity, inflammation | Every meal |
When to Involve Your Doctor

If you have implemented consistent lifestyle changes — improved nutrition, regular exercise, better sleep — and are still experiencing significant unexplained weight gain, a medical evaluation is the right next step.
Ask your physician specifically about:
- TSH (thyroid-stimulating hormone) — to rule out hypothyroidism
- Fasting insulin and fasting glucose — to assess insulin resistance and metabolic health
- Comprehensive metabolic panel — to evaluate liver and kidney function
- Hormonal panel — estrogen, progesterone, testosterone, and DHEA as appropriate
- Cortisol levels — especially if persistent fatigue, belly fat, and disrupted sleep are present
Weight management after 40 is not purely a matter of willpower. Biology matters enormously. And medical support can be the difference between years of frustration and genuine, sustainable progress.
Medical Disclaimer: The information provided in this article is for educational purposes only and is not intended to serve as medical advice, diagnosis, or treatment. Results may vary from person to person. If you have any medical conditions, are taking medications, or have health concerns, consult a licensed healthcare professional before making changes to your diet or health routine.
The Bottom Line: Your Body Changed, and Your Approach Needs to Match
Weight loss after 40 calls for understanding — and working with — a body that is genuinely different from the one you had at 25. Hormonal changes, muscle loss, insulin resistance, sleep disruption, and cortisol burden are not excuses. They are real physiological forces that require real, tailored strategies.
The same interventions that support weight management at midlife — resistance training, quality protein, restorative sleep, stress reduction, whole-food nutrition — also improve cardiovascular health, bone density, cognitive function, and overall quality of life. This was never only about the scale.
You are not broken. You are at a biological turning point — one that responds powerfully to the right approach. Small, consistent changes, applied with patience and self-compassion, build results that last.
Frequently Asked Questions
Why did I start gaining weight at 40 when my habits haven’t changed at all?
The most likely explanation is the compounding effect of gradual hormonal changes, slow muscle loss over time, and small metabolic shifts accumulating over years. What worked at 30 genuinely requires adjustment at 40 — not because you’ve failed, but because your physiology has changed. A basic medical workup to check thyroid function, hormones, and metabolic markers can clarify whether there’s an underlying driver.
Is it actually possible to lose weight after 40?
Absolutely — many adults lose meaningful weight and significantly improve their body composition after 40. The key is using strategies designed for a midlife body: adequate protein, progressive resistance training, sleep optimization, and stress management. Relying on caloric restriction alone, as many diets recommend, is rarely sufficient and can be counterproductive over time.
Does menopause make belly fat impossible to lose?
Menopause makes visceral fat accumulation more likely and harder to address — but not impossible. The hormonal shift toward abdominal fat storage can be meaningfully counteracted through consistent resistance training, an anti-inflammatory whole-food diet, quality sleep, and in some cases, a conversation with your doctor about hormonal evaluation. Many women see real improvements once their approach is aligned with their current hormonal reality.
Should I try intermittent fasting after 40?
Intermittent fasting can be effective for some adults over 40, particularly for managing insulin sensitivity and simplifying caloric intake. However, extended fasting can elevate cortisol and disrupt sleep quality if approached too aggressively. Women in perimenopause should be particularly cautious with prolonged fasting windows. Starting with a 12-hour overnight fast before considering extensions is a sensible, lower-risk approach.
How much protein do I actually need each day after 40?
Current research supports a protein intake of 1.2–1.6 grams per kilogram of body weight per day for active adults over 40. This is higher than standard dietary guidelines and reflects the increased protein needed to counteract age-related muscle loss. Prioritizing protein at breakfast in particular is associated with reduced appetite and better overall dietary adherence throughout the day.
Will eating very little just make my metabolism even slower?
Yes — severe caloric restriction below approximately 1,200–1,400 calories per day can trigger adaptive thermogenesis, in which your body deliberately reduces its energy expenditure to match dramatically reduced intake. This makes further weight loss progressively harder and increases the risk of muscle loss. A moderate, sustainable caloric deficit of 250–500 calories below your daily maintenance level, combined with resistance training, is far more effective over time.
Can chronic stress really cause weight gain even when I’m eating well?
Yes — and this is one of the most underappreciated realities of midlife weight management. Chronically elevated cortisol promotes visceral fat accumulation, amplifies appetite, drives cravings for calorie-dense foods, disrupts sleep, and undermines nearly every other weight loss strategy. For many adults over 40, stress management is not a peripheral concern — it is central to any lasting progress.







